Introduction
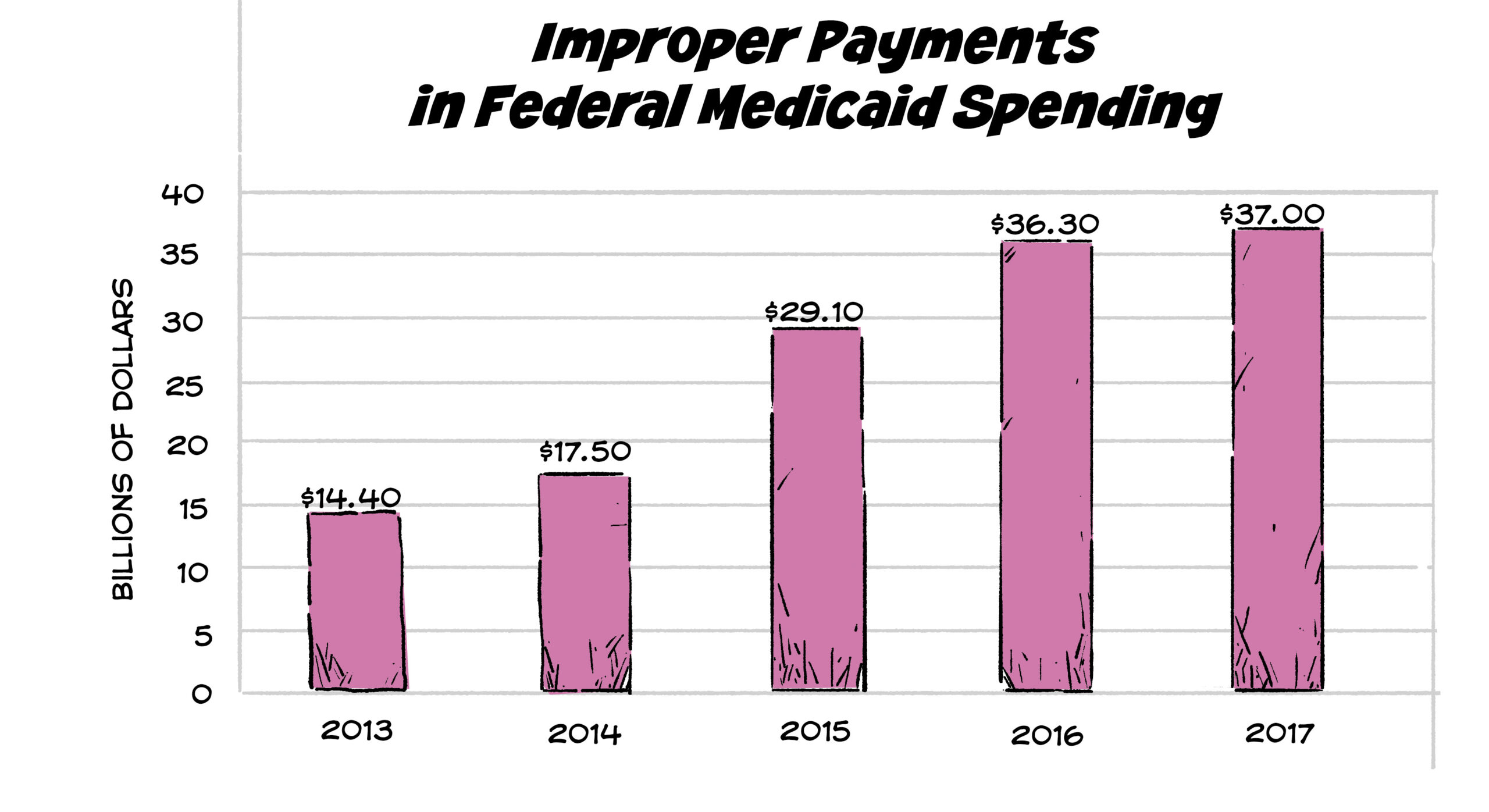
Improper Payments
In 2017 the Government Accountability Office (GAO) reported that Medicaid was responsible for one-quarter of all government-wide improper payments. These improper payments in Medicaid typically stem from overpaid, underpaid, or erroneous claims payments, amounting to a staggering $36.7 billion in wasteful spending. Every year for the past 15 years, this issue has landed Medicaid on the GAO’s high-risk list. Policymakers on both sides of the political aisle are very aware of the issue and are committed to tackling the fraud, waste,
and abuse in public health insurance programs. Finding better, more proactive ways to remedy Medicaid’s chronic problems with improper claims payments will save billions of taxpayer dollars. Syrtis Solutions (Syrtis) addresses this problem head-on and is a leader in the effort to reduce waste and help public health insurance programs function more efficiently.
Why Pay and Chase Has Been Normalized
It is important to note that improper payments are not the same as fraud. While there is fraud in Medicaid, and some improper Medicaid payments occur as a result, the two are very different. Instead, the vast majority of improper payments are made due to antiquated data systems and methodologies.
 There are many reasons why improper payments occur in government-funded health care systems:
There are many reasons why improper payments occur in government-funded health care systems:
Coordinating benefits and determining third party liability (TPL) is complex, requiring timely data and the management of multiple data sources
The Medicaid population has a high rate of churn and is in near-constant flux
Eligibility data is not coordinated between federal and state systems and is often inaccurate
By law, Medicaid plans are payers of last resort. This means if a beneficiary has health care coverage through any other third party, that third party must pay its legal liability first. If any liability remains, Medicaid plans will then pay. According to the Centers for Medicare and Medicaid Services (CMS), “States are required to take all reasonable measures to ascertain the legal liability of third parties to pay for care and services that are available under the plan.”
This policy has been in place since the Employee Retirement Income Security Act (ERISA) amended the Social Security Act in 1974. To this day, ascertaining TPL remains a difficult challenge. Coordination of benefits (COB) is no easy task. CMS explains that COB is accomplished by, “determining Medicaid benefits when an enrollee has coverage through an individual, entity, insurance, or program that is liable to pay for health care services.”
How TPL is Identified on Medicaid
The discovery of liable third parties occurs at three points in the lifecycle of a Medicaid member. This discovery of unknown primary insurance coverage may occur during the enrollment process, prospectively before claims are paid, and retrospectively after an improper claims payment has been made (pay and chase).
In the enrollment phase, Medicaid applicants are approved and their self-reported TPL is verified and reported to the state. The main challenge is that over 13% of the Medicaid population has unreported TPL. Applicants are often unaware of other coverage or fail to disclose it at the time of enrollment. At the point of service – when members are presenting insurance information to care providers – they might not furnish proof of primary coverage. The system is certainly complex, and Medicaid members may not realize that they have valid primary coverage, and even if they do, it is doubtful that they are familiar with the concept of payers of last resort. Compounding the confusion, the Medicaid population is in near-constant flux, with people becoming eligible and ineligible for services depending on a number of factors such as income and disability status.
Once an applicant is enrolled, Medicaid plans attempt ongoing prospective identification of other insurance coverage. The challenges here are the same issues that are responsible for the high number of improper payments in the Medicaid program. That is, existing data mining and matching models are antiquated and need constant verification. Sometimes, a Medicaid plan uses an outside vendor to conduct monthly eligibility checks in an attempt to discover a Medicaid member’s TPL. Unfortunately, the data available to these vendors
suffer the same antiquation and inaccuracy problems. Though health plans try to discover TPL in as timely a manner as possible, there are many obstacles.
The final point at which health plans can discover TPL is retrospectively after claims are paid in error. At present, pharmacy and medical claims reviews are profoundly retrospective, which creates a multitude of problems for improper payments. Consequently, a post-payment recovery process, know as ‘pay and chase,’ is needed to recoup the claims payments that were made in error. Beyond simple mistakes at the point of service with providers, there are fundamental problems in the health care data utilized by the federal government that lead to the loss of literally billions of dollars a year.
One of the major challenges facing Medicaid is the lack of quality eligibility data. In testimony before Congress in 2012, HHS Regional Inspector General Ann Maxwell gave an alarmingly negative assessment regarding the reliability of data the federal government uses to detect overpayments and fraud in the Medicaid program. She stated, “much of the data used to identify improper payments and fraud is not current, available, complete, [or] accurate.”
3 See Medicaid and State Children’s Health Insurance Program (CHIP) Payment and Access Commission, Report to the Congress on Medicaid and CHIP, March 2014 (Washington, D.C.: March 14, 2014).

Why Pay and Chase Has Been Normalized
 Without reliable, complete, and accurate data, Medicaid plans often make claims payments in error, leading to one common course of action: “pay and chase.”
Without reliable, complete, and accurate data, Medicaid plans often make claims payments in error, leading to one common course of action: “pay and chase.”
The ability to identify liable third party payers before claims are improperly paid has been a chronic challenge due to:
Antiquated technology
Siloed data systems
Network latency
“Pay and chase” occurs when:
Payments are made in good faith by a payer of last resort.
That payer later discovers the payments were made in error and were actually the responsibility of another third party payer.
The payer of last resort then attempts to recoup the funds from the responsible third party payer.
Because of unreliable eligibility data, Medicaid plans frequently pay claims that are not, in fact, their responsibility. When new eligibility information or updated data becomes available and plans uncover overpayments, the “chase” begins.
Federal payer of last resort programs such as Medicaid have been allowed to pay claims in error and pursue reimbursements for two primary reasons. First, CMS has widely approved waivers to the cost avoidance directive. Second, there is an obvious need to recover claims payments when third party liability (TPL) is identified retrospectively.
The practice of ‘pay and chase’ has become normalized, even though cost avoidance and routing claims to the proper payers is the only way to ensure federal dollars are not paid in error. Furthermore, an entire multi-billion-dollar industry has been built around post-payment recovery. Unfortunately for payers trying to recoup improper claims payments, the actual funds recovered remain around twenty cents on the dollar.
On another, practical front, it is understandable that plans may sometimes pay so as not to drag out the claims payment process. When coordinating benefits causes claims payments to be delayed, providers become dissatisfied, and this could result
in providers choosing not to participate in Medicaid.5 There is already a shortage of providers willing to accept Medicaid, so rather than exacerbate this problem; Medicaid plans pay, even if it means they will have to chase those dollars later.
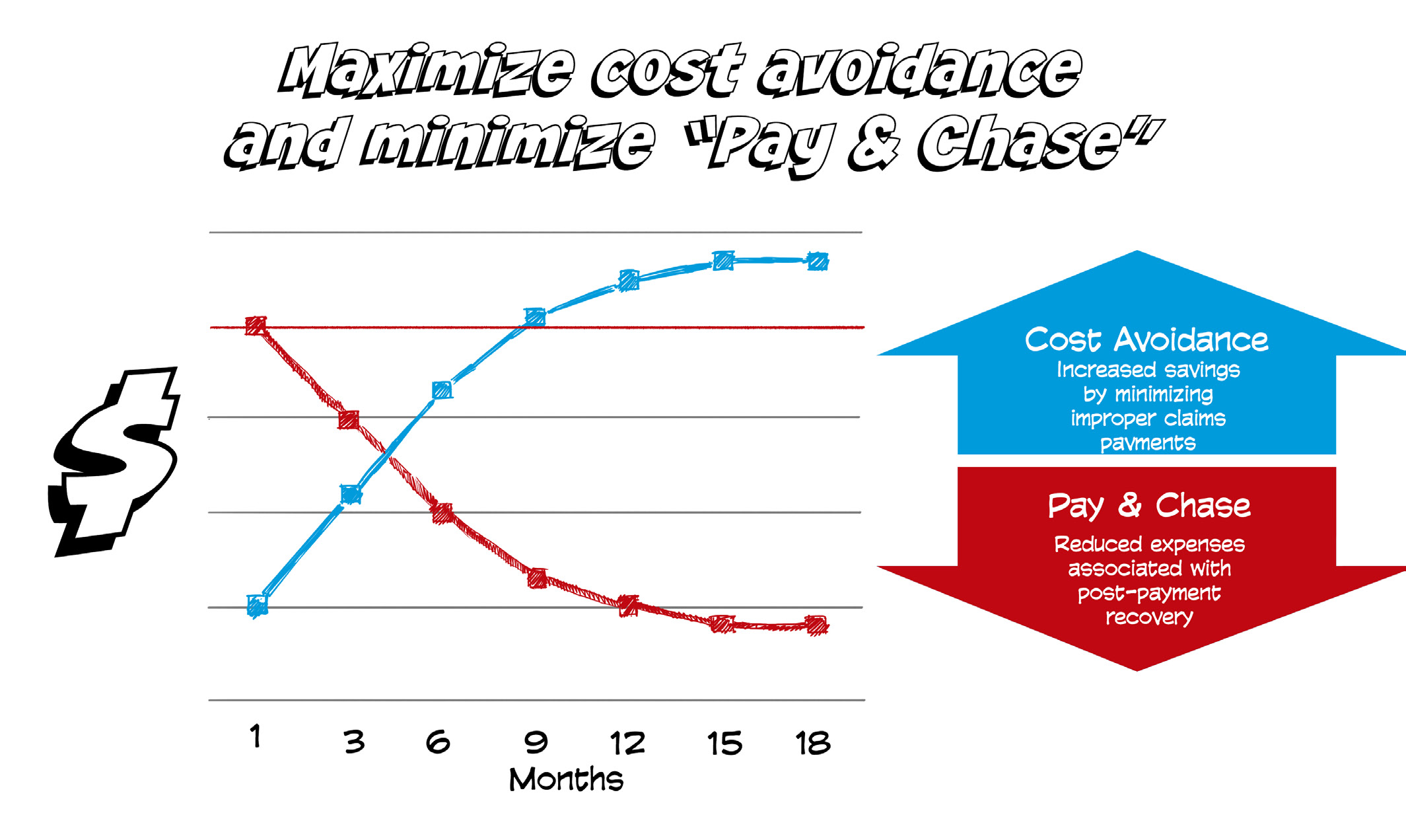
Cost Avoidance vs ‘Pay & Chase’
Cost avoidance is more efficient than ‘pay and chase,’ plain and simple. If payers of last resort can identify whether a plan member has primary coverage, before claims are paid, the need for post-payment recovery is miti-gated. While improper payments may never be eliminated completely, employing a suite of technology solutions along the payment continuum can help Medicaid plans maximize the efficiency of their adjudication processes.
The subset of Medicaid members who have unreported primary commercial coverage present a tremendous opportunity for payers of last resort to “get in front” of the problem. With the timely delivery of accurate eligibility data on these members, improper claims payments and wasteful spending can be limited.
- Cost avoidance is more efficient than ‘pay and chase’
- A suite of technology solutions along the payment continuum
helps Medicaid plans maximize claims payment efficiency - CMS is working to improve and unify state Medicaid data
- EPrescribing data are accessible, accurate, and available for Medicaid plans to utilize for the identification of TPL
How to Get Better Data and Become More Efficient
Therefore, the question becomes: how can payers of last resort get access to timely, accurate eligibility data? Currently, eligibility data are housed in massive data repositories, and the data are mostly stale, old, and unusable. The state Medicaid Management Information Systems (MMIS) around the country are disparate and siloed. The Transformed Medicaid Statistical Information System (T-MSIS), is CMS’s attempt to bring all these disparate systems together, but it is years from completion. According to CMS, this new, more unified dataset includes, “enhanced information about beneficiary eligibility, beneficiary and provider enrollment, service utilization, claims and managed care data, and expenditure data for Medicaid and CHIP.”
CMS has also tried to improve Medicaid payment errors by creating the Public Assistance Reporting Information System (PARIS) Medicaid Interstate Match. The Medicaid population is not only constantly in flux relative to its eligibility for the program, but also in terms of its residency. CMS found that beneficiaries crossing state lines were one source of improper payments because a mechanism did not exist for states to share information and “match” beneficiary information.
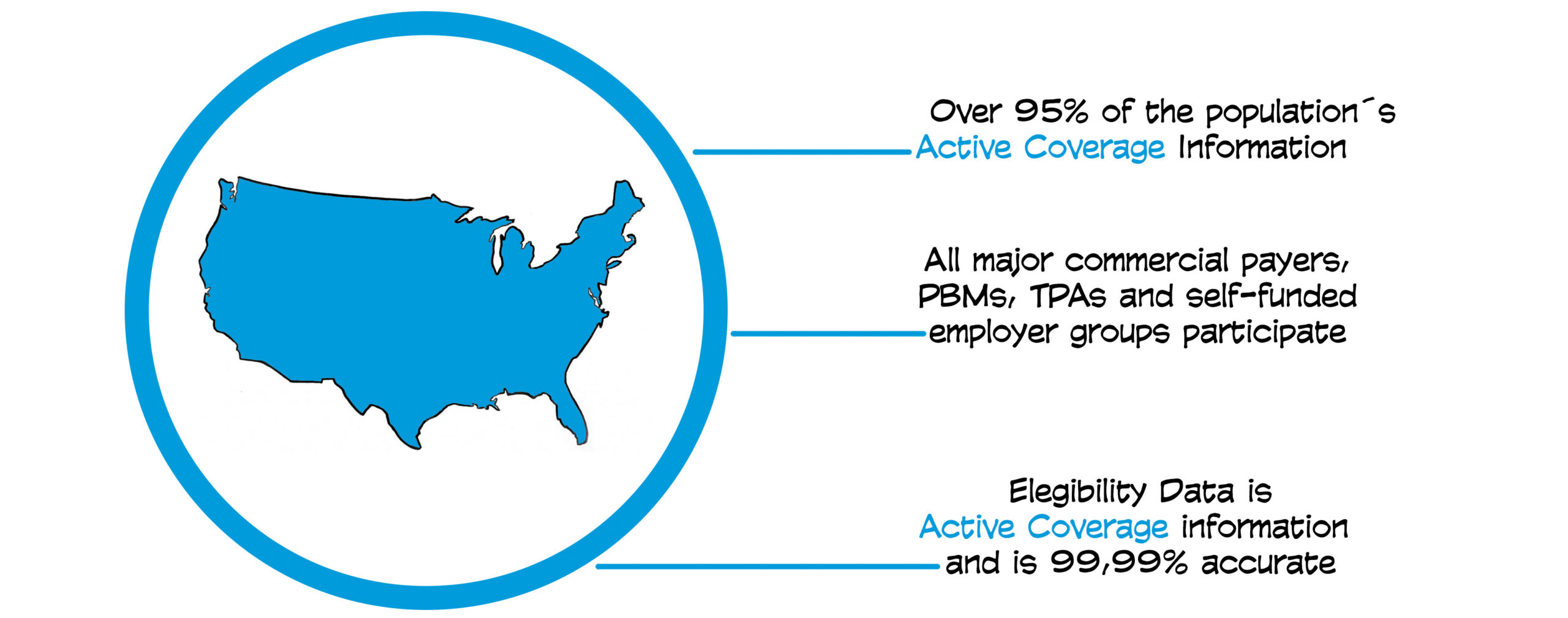
While federal efforts to improve data sharing nationwide are important, these efforts are ongoing. Right now, some of the best, most accurate data on patients’ health insurance coverage reside in ePrescribing infrastructures. Leveraging this resource allows for more timely identification of TPL; it captures the necessary information on primary coverage that Medicaid members may have. EPrescribing information is also secure. It electronically connects patients, providers, pharmacies, and pharmacy benefits managers and ensures patient eligibility data is accurate and up to date.
- Federal efforts to improve nationwide data sharing
- Access to ePrescribing data for timely, accurate TPL discovery
- Find and maintain data for members who utilize their benefits
instead of entire Medicaid populations
Benefiting from Expertise and Experience
Medicaid plans agree that cost avoidance makes more sense, but until now the ability to execute it effectively has not been widely available. Through Syrtis, ePrescribing data can be delivered in a timely fashion, and it is useful because it is accurate and delivered quickly. Payers of last resort are acting on this data with confidence.
Part of the efficiency of this solution is that it allows health plans to target utilizers of health care services, those generating claims. Currently, Medicaid plans attempt to maintain – or at least obtain – data on every Medicaid plan member. Now, they can use an as-needed approach, receiving data as the need arises.
Syrtis is the only provider of primary commercial pharmacy and medical coverage data obtained through an ePrescribing master patient index (MPI), a solution known as ProTPL. Studies have demonstrated that up to 80% of the other health insurance (OHI) discovered via the ProTPL methodology cannot be found using any other existing process. 8 Payers of last resort that utilize ProTPL achieve up to a 40% increase in discovery of primary payers (above and beyond any TPL processes). Once deployed, ProTPL immediately mitigates improper claims payments and the need for ‘pay and chase.’

Syrtis, with its vast experience in pharmacy operations and National Council for Prescription Drug Programs (NCPDP) standards, is the only vendor in the marketplace with the proprietary logic necessary to decipher the complex coding of pharmacy transactions and translate it into actionable eligibility data that can be utilized by payers of last resort to cost-avoid improper prescription and medical claims payments. Furthermore, Syrtis uses its superior matching algorithm to find primary coverage on members that no other vendor in the marketplace can find.
EPrescribing data certainly was not originally intended for these purposes. However, its potential to yield significant “low-hanging fruit” in the battle against improper payments is undeniable. This is not just another recovery program. It addresses the problem of improper payments on the front end, gathering better data and applying them so as to avoid claims costs and the expenses associated with recovery efforts. This has the added benefit of making the claims process smoother for all involved, including providers. Those involved in
the process of Medicaid claims payments have been operating with the best tools they had available. Now, they have new and better tools through Syrtis.